Magnetic resonance imaging for lung cancer: a state-of-the-art review
Article information
Abstract
Lung cancer is the leading cause of cancer-related deaths worldwide, and imaging techniques such as chest radiography, computed tomography (CT), positron emission tomography (PET), and magnetic resonance imaging (MRI) play an important role in its diagnosis, staging, treatment planning, post-operative surveillance, and treatment response evaluation. Pulmonary MRI can non-invasively visualize structural and functional abnormalities in the lungs without using ionizing radiation, although it has been suggested that it has less clinical utility than chest radiography, CT, and PET/CT for thoracic diseases, especially lung diseases. With recent advances related to MRI pulse sequences, pulmonary MRI has become practicable in an expanding number of clinical situations. This review article focuses on recent advances in MRI and discusses its clinical applications in the detection, diagnosis, staging, pre-operative evaluation, post-operative surveillance, and treatment response evaluation of lung cancer.
INTRODUCTION
Lung cancer is a leading cause of cancer-related morbidity and mortality worldwide [1], and imaging techniques such as computed tomography (CT) and positron emission tomography (PET) play an important role in its diagnosis, staging, treatment planning, post-operative surveillance, and treatment response evaluation [2]. Although it has been suggested that magnetic resonance imaging (MRI) has less clinical utility for thoracic diseases than radiography, CT, and PET/CT, for certain specific indications, MRI has recently become more practicable owing to advances in post-processing software and analysis methods, magnetic resonance (MR) pulse sequences, multi-coil parallel imaging and acceleration methods, and the use of contrast media. Moreover, various functional and metabolic sequences and morphological sequences to enhance relaxation time differences introduced since 2000 have been found to be of considerable clinical relevance in cancer as well as other diseases. Thus, MRI for thoracic diseases is currently an attractive research field and represents a new frontier in MRI technology. In this article, we review both basic and advanced MRI techniques and discuss their clinical applications for lung cancer.
THORACIC MRI TECHNIQUES
Paul Lauterbur, who received the 2003 Nobel Prize in Medicine with Peter Mansfield, developed the first MRI scanner in the 1970s. Inhomogeneity in magnetic susceptibility due to air and soft tissue interfaces within the lung, combined with motion and low intrinsic proton density, hinders the use of MRI in the lung parenchyma [3-11]. Moreover, differences in susceptibility to artifacts in the lung parenchyma and chest wall manifest as a dark line perpendicular to the frequency encoding direction. Therefore, thoracic MRI was initially considered less informative than CT for the assessment of lung parenchymal diseases and thoracic oncologic diseases in clinical practice [4,6,8-33]. Nonetheless, researchers have been trying to enhance the utility of MRI for lung cancer and mediastinal tumors and for pulmonary vascular diseases [4,6,8-33].
Traditional MRI for lung cancer
In the early 1990s, spin echo (SE) sequences were used for clinical lung cancer MRI; however, reports published by the Radiologic Diagnostic Oncology Group concluded that MRI with non-electrocardiogram (ECG)-gated T1-weighted SE imaging had less utility than CT for tumor, lymph node, and metastasis (TNM) staging [34]. Since then, continuous and remarkable technical advancements have been made. Techniques such as turbo or fast SE and gradient-recalled-echo (GRE) sequences, fast GRE with short echo time (TE), in- and opposed phase T1-weighted GRE, T1- and T2-weighted, short inversion time inversion recovery (STIR), and turbo spin echo (TSE) with the half-Fourier single-shot method with and without black-blood have been used in routine clinical practice since the early 1990s [6,10,11,13,17,20,24-26,29]. Diffusion-weighted imaging (DWI) has been used in combination with single-shot echo-planar imaging (EPI) sequences and the fat-suppression technique for oncologic evaluation since the early 2000s [13,17,20,24-26,29]. Therefore, almost all MRI sequences forthoracic oncological diseases were established by the mid-2000s. During the same period, the parallel imaging technique, as well as fast GRE with short TE or ultrashort TE (UTE) and contrast media were proposed for time-resolved (or 4D) contrast-enhanced (CE-) MR angiography, dynamic CE (DCE-) MRI, and DCE-perfusion MRI; assessments of these techniques have demonstrated that they are clinically relevant for the management of pulmonary nodules and masses and for TNM staging [6,10-13,16,17,20,22-26,28-31]. Since the mid-2000s, even newer techniques for dedicated thoracic MRI and whole-body MRI have been introduced and used for morphological and functional evaluation. Recently, a PET technique using 18F-fluorodeoxyglucose (FDG) with MRI (FDG-PET/MRI or FDG-MR/PET) has been developed, and attempts have been made to evaluate MR-based and glucose metabolism-based information simultaneously [24]. Moreover, MRI techniques have started being used as molecular imaging tools [35,36].
Technical advances in MRI during the past decade
The clinical availability of 3T MRI has increased. The high-field strength increased the signal-to-noise ratio (SNR) and resolution, which improved lesion detection; however, for the lungs, susceptibility and image distortion are more severe on 3 T MR than on 1.5 T MR images due to magnetic field inhomogeneity [13,37,38]. Fink et al. [37] showed that the imaging characteristics of different pulse sequences for lung MRI were similar at 1.5 and 3 T, but that higher lesion contrast can be expected at 3 T. In addition, T1-weighted 3D turbo field echo and T2-weighted triple-inversion black-blood TSE 3 T MRI allow the detection of clinically significant pulmonary nodules nearly as well as CT [39]. On the other hand,the performance of low-field MRI systems has been considered poor, with limited spatial resolution and low SNR [40]; nevertheless, Campbell-Washburn et al. [38] reported that a low-field MRI system equipped with high-performance image technology could reduce distortion by reducing susceptibility and deliver excellent image quality because of improved field homogeneity.
Since the early 2000s,DWI has been applied as a form of MRI that measures the random Brownian motion of water molecules within a voxel of tissue. Diffusion is particularly useful in tumor characterization, N- and M-stage evaluation, and therapeutic effect prediction [13,17,20,24-26,29,41-47]. Although the most commonly used technique relies on SE-EPI, non-EPI techniques such as fast advanced SE or TSE are also available and useful for lung cancer evaluation using high-field MR, especially 3 T MR, systems to reduce image distortion and improve image quality and accuracy of apparent diffusion coefficient(ADC) measurements [48,49].
DWI allows the calculation of tissue ADC, a quantitative measure of tissue diffusivity, and enables the objective comparison of results for pulmonary mass characterization, N- and M-stage assessments, predicting the therapeutic effects of conservative therapy, and evaluating treatment response after chemotherapy in non-small cell lung cancer (NSCLC) [13,17,20,24-26,29,41-47,49]. However, signal attenuation on DWI at low b-values (e.g., 0 to 100 sec/mm2) arises not only from water diffusion in tissues, but also from microcirculation within the normal capillary network [41-53]. In 1986, Le Bihan et al. [54] termed the behavior of protons that display signal attenuation on DWI intravoxel incoherent motion (IVIM), and suggested that using more sophisticated approaches to describe signal attenuation in tissues with increasing b-values would enable the estimation of quantitative parameters that separately reflect tissue diffusivity and tissue microcapillary perfusion [55]. Using IVIM-based analysis, it is now possible to derive other quantitative indexes that describe tissue water diffusivity (slow component of diffusion), tissue perfusion (pseudo diffusion coefficient), and tissue perfusion fraction.
Spoiled 3D GRE sequences with different fat-suppression techniques—such as 3D volumetric interpolated breath-hold examination (VIBE; Siemens Healthineers, Erlangen, Germany), T1-weighted high-resolution isotropic volume examination (THRIVE; Philips Healthcare, Cambridge, MA, USA), and the fast and segmented 3D T1-weighted spoiled gradient echo sequence (Quick 3D, Canon Medical Systems, Otawara, Japan)—have replaced T1-weighted SE and TSE sequences for obtaining CE-T1-weighted images in lung cancer, and are in clinical use for nodule detection in thoracic MRI, TNM stage evaluations and recurrence assessments in whole-body MRI, and FDG-PET/MRI in NSCLC [56-59].
Since the mid-2010s, radial acquisition of k-space data from free induction decay has reduced TE to less than 200 μs, minimizing signal decay due to a short transverse relaxation time (T2/T2*). It has therefore been suggested that the development of UTE or zero TE sequences could be a game changer for thoracic MRI [4,6,8-11,13,22,60-64], because they would allow for better visualization of endogenous lung parenchyma MR signal than with conventional short echo image sequences. MRI with UTE could also enable quantitative assessment of regional T2* values and morphological changes in pulmonary parenchymal diseases [60,63]. Therefore, MRI with UTE could enable new morphological MRI assessments not only for thoracic oncology but also for other pulmonary diseases.
As a new molecularimaging method using magnetic fields equal to or higher than 3 T, chemical exchange saturation transfer (CEST) imaging maps the chemical exchange between bulk water protons and exchangeable protons in small metabolites and macromolecules [35,36,65,66]. The most commonly studied signals in CEST imaging arise from the amide proton transfer signals of peptides and proteins, called amide proton transfer (APT) imaging. This new technique has been tested for nodule characterization, and its clinical potential has been suggested in a few studies [35,36].
CLINICAL APPLICATIONS OF THORACIC MRI
Lung nodule detection and lung cancer screening
Since 2011, annual screenings using low-dose computed tomography (LDCT) have been performed worldwide, as this can reduce lung cancer mortality by 20% [67], with the CT-based Lung Imaging Reporting and Data System (Lung-RADS) being widely used for nodule assessment and subsequent management [68]; however, this increases radiation burden and can lead to unnecessary invasive procedures or complications, because LDCT has a high malignancy-related false-positive rate (23%) [67].
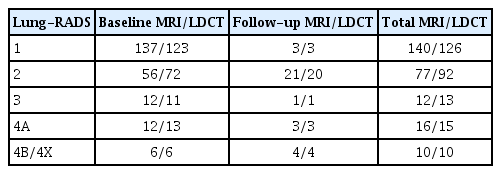
MRI has been perceived to be inferior to CT in evaluating small nodules because of its sensitivity to cardiac and respiratory motion artifacts, very low T2* values, lung magnetic field heterogeneity, and low proton density of the lung parenchyma [69]. However, techniques using three-dimensional GRE and UTE sequences and thin-section thicknesses (1 to 1.25 mm) have shown detection rates of more than 90% for lung nodules ranging from 4 to 29 mm in diameter, which is at least as efficacious as standard- or reduced-dose thin-section CT for nodule detection [61,62]. Although study results have varied because of the use of different hardware and software settings, the ability of MRI to detect solid nodules was 57.1% for nodules smaller than 4 mm, 60% to 90% for nodules 5 to 8 mm, and almost 100% for nodules 8 mm or larger[70-74]. MRI under the optimal conditions of successful breath-holds and reliable gating or triggering detected 90% of 3-mm nodules [75], and MRI with spiral UTE sequences had a 95% success rate regardless of nodule size [76]. Nodule detection rate using spiral UTE sequences was >65% for non-solid nodules (3 to 20 mm), >75% for part-solid nodules (5 to 18 mm), and 100% for nodule size >16 mm [76]. MRI using the pointwise encoding time reduction with radial acquisition sequence on a 3 T system detected 72% and 94% of <3-cm ground glass and part-solid nodules,respectively (Table 1) [70-74,76,77]. Discrimination of attenuation of detected nodules by MRI indicated almost perfect agreement compared to that with CT [77]. The average risk of cancer in solid nodules smaller than 6 mm in high-risk patients is less than 1% [78]; as nodules >8 mm require short-term follow-up or further evaluation according to the Lung-RADS [68], it is reasonable to evaluate the use of MRI to screen for lung cancer. In a recent study, Meier-Schroers et al. [79] compared LDCT- and MRI-derived Lung-RADS categories in two screening rounds. Nodules from 224 participants were prospectively analyzed following the German Lung Cancer Screening Intervention Trial inclusion criteria using LDCT and T2, balanced T1, and DWI MRI sequences at 1.5 T. Nodule size detected using MRI correlated significantly with the LDCT findings; MRI accurately detected 70% of solid nodules <6 mm, 98% of solid nodules ≥6 mm, and 72% sub-solid nodules <20 mm in size (Fig. 1). Moreover, the MRI and CT Lung-RADS score correlated significantly, and nodules with a Lung-RADS score of 3 or more were never under-scored or missed using MRI (Fig. 2), although MRI-based Lung-RADS scores were overestimated in terms of size and presence of pulmonary vessel or streaky opacities, and underestimated for 4 to 5 mm solid nodules and sub-solid nodules smaller than 20 mm (Table 2). The early recall rate decreased from 13.8% at baseline to 1.9% during the second screening, consistent with the indicator of good quality based on hypothesized optimal recall for mammographic examinations (12% to 14%) [80].

Results from prior publications regarding the diagnostic performance of various MRI sequences in terms of nodule detection and determination of malignancy

A 10 mm solid nodule in the left upper lobe in a 58-year-old man. The nodule (arrows) was clearly visible using all magnetic resonance imaging (MRI) sequences and classified as Lung-RADS 4X because of a spiculated margin. (A) Computed tomography (CT) lung window, (B) CT soft tissue window, (C) MRI T2 short inversion time inversion recovery, and (D) MRI contrast-enhanced fat-saturated T1-weighted images.
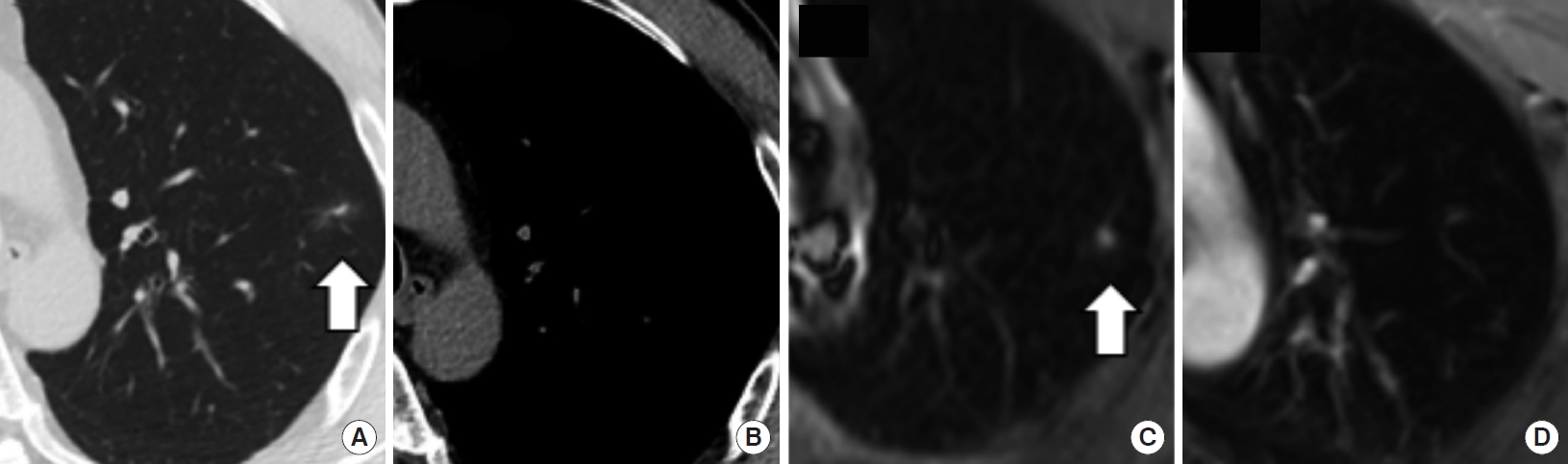
A 12 mm sub-solid nodule in the left upper lobe (classified as Lung-RADS 2 based on magnetic resonance imaging [MRI] and computed tomography [CT]) in a 58-year-old man. This nodule (arrows) was only slightly hyperintense on T2-weighted sequence images and hardly detectable using contrast-enhanced fat-saturated T1-weighted imaging. (A) CT lung window, (B) CT soft tissue window, (C) MRI T2 short inversion time inversion recovery, and (D) MRI contrast-enhanced fat-saturated T1-weighted images.
Concerning false-positives in lung cancer screening using LDCT, another study that compared MRI and LDCT for lung nodule detection in a high-risk population reported a 5% false-positive rate using MRI [81], which was better compared to that in the first round of the National Lung Cancer Trial (23.3%).
Thus, several studies show that lung MRI could be a potentially effective screening tool, with a performance comparable to that of LDCT, but with a lower false-positive rate and no radiation exposure.
Lung nodule characterization
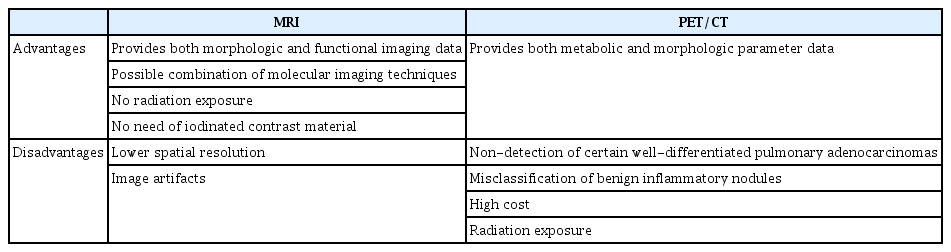
Since pulmonary nodules are one of the most common chest imaging findings, it is important to differentiate between malignant and benign nodules. Although CT is the most widely used modality for pulmonary nodule evaluation, it relies on morphological examination and contrast enhancement, resulting in is high sensitivity (95% to 100%) but relatively low specificity (30% to 58%) [82]. PET/CT performed using the radiotracer 18FDG is also a useful tool. It combines both metabolic and morphologic parameters for nodule characterization [83,84]; however, there are some disadvantages, such as non-detection of some well-differentiated pulmonary adenocarcinomas, misclassification of benign inflammatory nodules, high cost, and radiation exposure (Table 3) [85-87].
Numerous MRI sequences have been evaluated for pulmonary nodule characterization [28]. To date, DWI is considered the most useful tool in this regard—many studies have shown that cancerous lung nodules have significantly higher signals on DWI and lower signals on ADC maps than benign ones (sensitivity, 70% to 99%; specificity, 66% to 97%) [42,88-93]. Moreover, when efficacy was compared with that using 18FDG in PET/CT,the results were satisfactory [88,93]. Table 4 shows the major study results regarding pulmonary nodule diagnosis using DWI. Image distortion remains a major limitation, but emerging techniques may be able to correct this. Correcting distortion using reverse-phase encoding diffusion-weighted 3 T PET/MRI showed satisfactory results in reducing ADC value errors when evaluating lung tumors [94]. A few studies have attempted to evaluate the utility of DCE-MRI in diagnosing lung nodules with a focus on management, showing that DCE-MR indexes were useful in differentiating between solitary pulmonary nodules that necessitated further evaluation or treatment (malignant or actively infected) and nodules that did not(benign) [95,96].
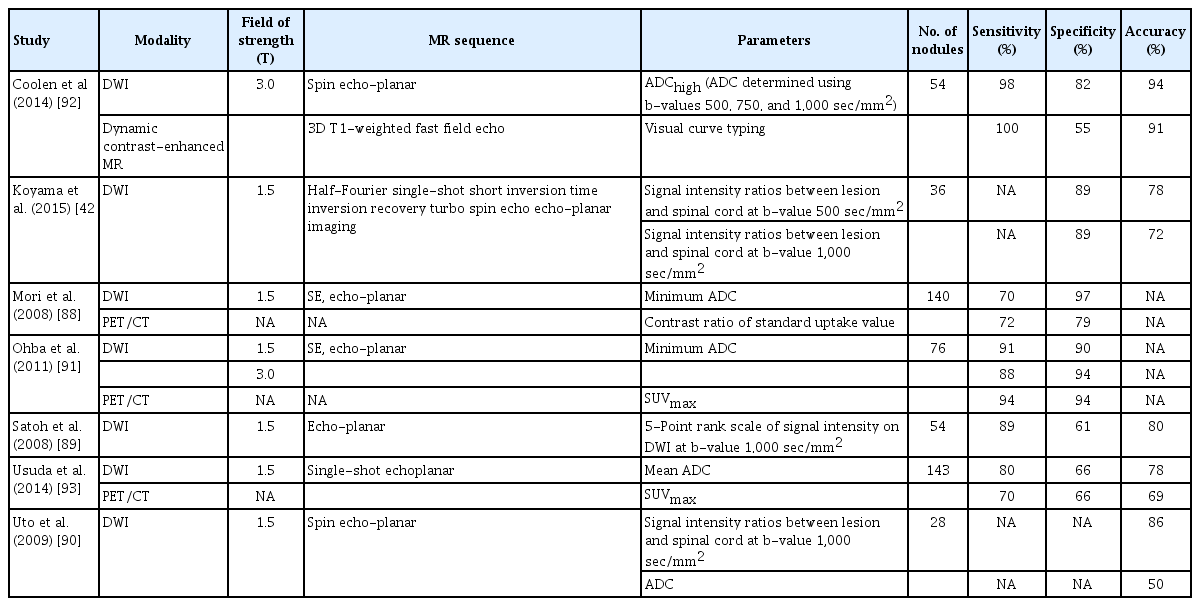
Diagnostic performance of diffusion-weighted MRI in terms of distinguishing between malignant and benign pulmonary nodules
MRI has clear advantages in certain clinical situations, such as differentiating lung cancer from progressive massive fibrosis (PMF), tuberculomas, or obstructive pneumonia—when T2-weighted MRI was used to study PMF in 24 patients with coal workers’ pneumoconiosis, signal intensity of PMF was low, whereas most lung cancer lesions showed intermediate or high signal intensity (Fig. 3) [97]. Tuberculoma lesions tend to have a more heterogeneous signal intensity than lung cancer lesions, and a higher percentage of tuberculosis lesions have hypo-intensity on T2-weighted images and hyperintensity on T1-weighted images [98]. CE imaging can differentiate tuberculomas from lung cancer, because tuberculomas frequently show a thin enhancing rim and a non-enhancing central zone on post-contrast MRI, which correlates with the histological findings that tuberculomas have a fibrous peripheral capsule and epithelioid granulomas in the central zone [99].
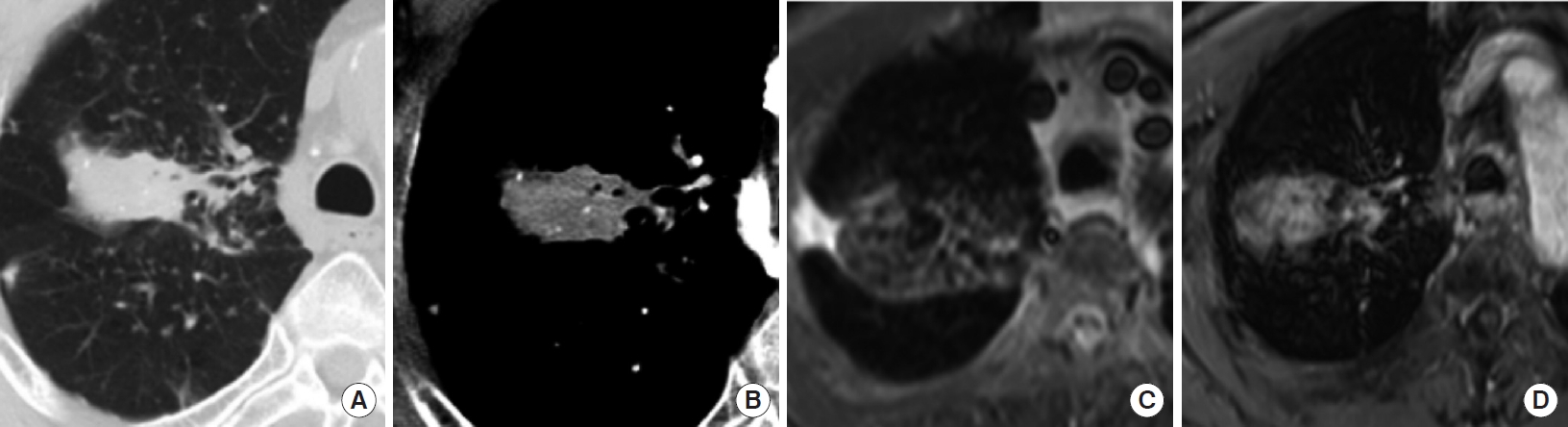
Case of an 81-year-old man with progressive massive fibrosis (PMF) confirmed based on percutaneous biopsy. (A) Thin-section computed tomography (CT) image showing a well-defined mass in the right upper lobe. Multiple small nodules indicative of pneumoconiosis are also seen in the surrounding lung tissue. (B) The mass has an inhomogeneous enhancement pattern on contrast-enhanced CT. Differentiating PMF from lung cancer on the basis of CT findings was difficult. (C, D) The main nodule showed very low signal intensity on T2-weighted magnetic resonance imaging (MRI) (C) and a heterogeneous enhancement pattern on contrast-enhanced T1-weighted MRI (D), which indicated that PMF was more likely than lung cancer.
MRI also enables accurate delineation of tumors from surrounding post-obstructive atelectatic areas, which is important for therapy planning. In some cases, it can be difficult to distinguish between lesions and regions of post-obstructive atelectasis or pneumonitis, because these secondary changes and the tumor tend to be enhanced to a similar degree on CE-CT. On T2-weighted or CE-T1-weighted images, however, post-obstructive atelectasis and pneumonitis often have a signal intensity distinct from that of tumors [100,101], possibly due pulmonary vasculature invasion. Furthermore, researchers have reported that post-obstructive atelectasis ADC value appears to be higher than those of lung tumors (Fig. 4) [102,103].
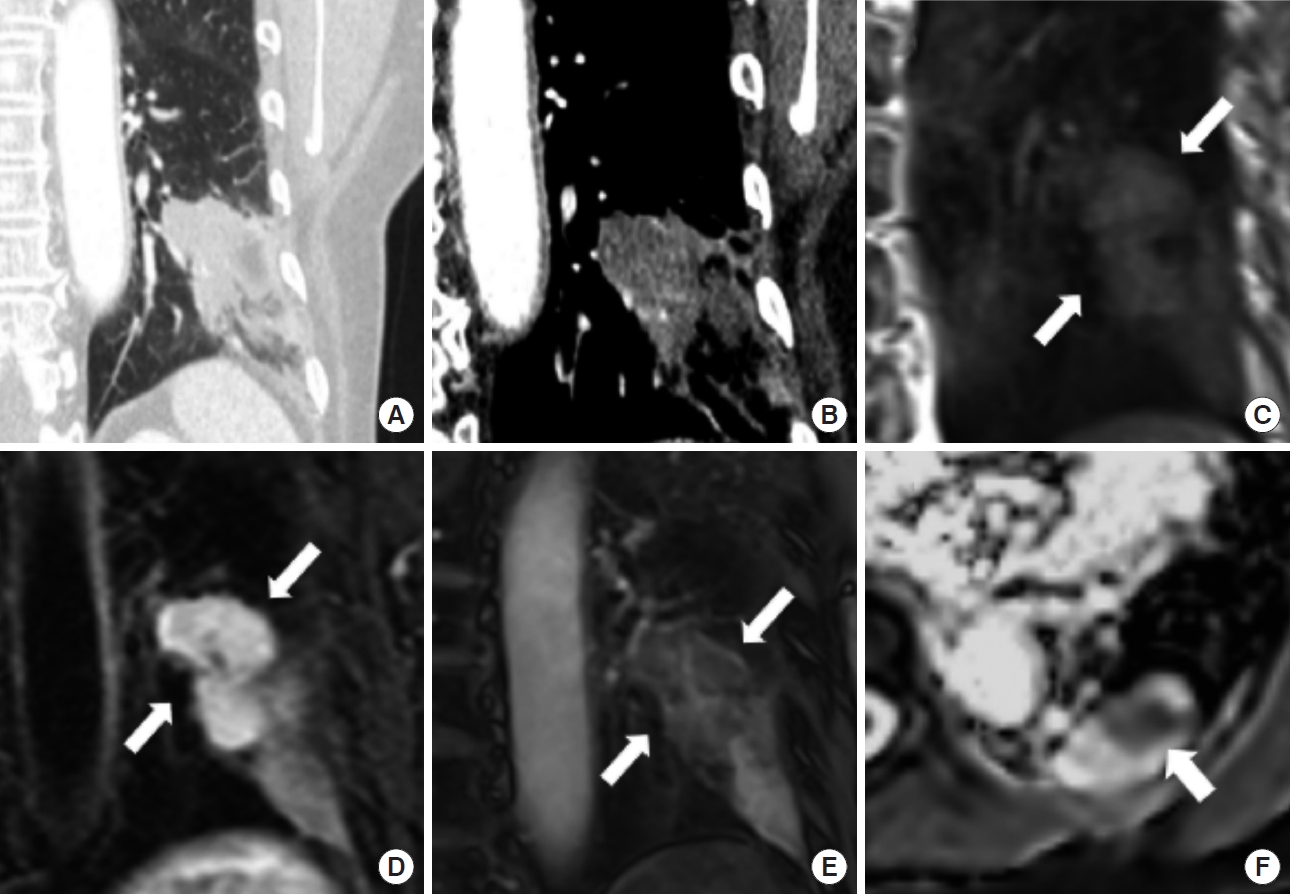
Case of a 70-year-old female with adenocarcinoma. (A) Thin-section computed tomography (CT) shows a tumor with distal atelectasis in the left lower lobe. (B) Contrast-enhanced thin-section CT shows homogenous enhancement in the tumor and the atelectatic region, but the extent of the tumor cannot be accurately determined. (C) Black-blood T1-weighted magnetic resonance imaging shows the tumor (arrows) and distal atelectasis as regions of intermediate and low signal intensity, respectively. (D) T2-weighted images show the tumor (arrows) and atelectasis as regions of high and intermediate signal intensity, respectively. (E) A post-contrast T1-weighted image clearly showing the extent of the tumor (arrows) and secondary atelectasis. (F) In the apparent diffusion coefficient (ADC) map, the mean ADC value of the tumor (1.341×10−3 mm2/sec) (arrow) was lower than that of the surrounding atelectatic region (2.947×10−3 mm2/sec).
Recent studies have focused on the potential of MRI-based imaging biomarkers that can stratify the risk in lung cancer patients. As DWI can provide information about tumor cellularity, investigators have attempted to differentiate lung cancer subtypes using ADC values. Differences in ADC values have been reported for small cell lung cancer and NSCLC [104,105]—ADC values in the former were lower, probably due to histologic factors such as high cellularity tumors with large nuclei and almost no cytoplasm, which reduce diffusion-based motion [106]. Among the NSCLCs, adenocarcinoma ADC value was significantly higher than that of squamous cell carcinoma (Figs. 5, 6) [105]. Mucinous adenocarcinomas, which have characteristic mucin production, in particular tend to have significantly higher ADC values than other types (Fig. 7) [93,105]. Lee et al. [107] showed that mean ADC values correlate well with lung adenocarcinoma histologic grades, and Kanauchi et al. [108] reported that DWI might be useful for predicting the invasiveness of stage IA NSCLC.
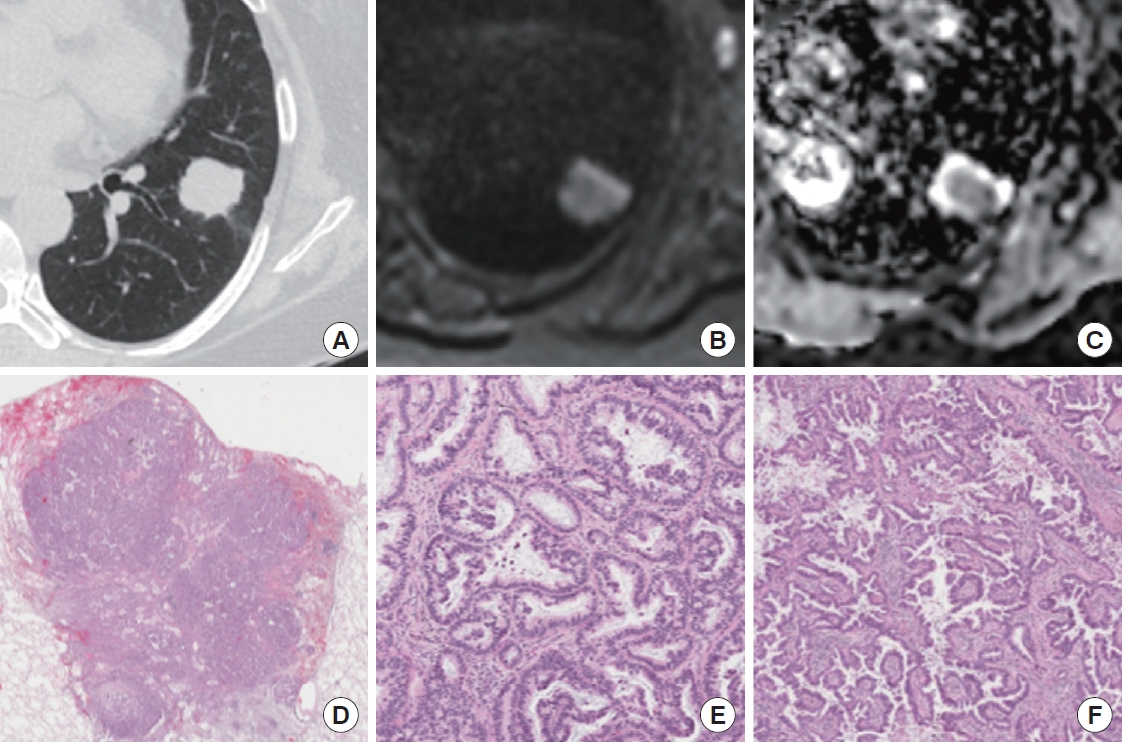
Case of 63-year-old female with adenocarcinoma in the left lower lobe. (A) Conventional computed tomography shows a lobulated nodule in the left lower lobe. (B) Diffusion-weighted imaging (b-value=700) shows a high signal. (C) The mean apparent diffusion coefficient of the carcinoma was 1.300×10−3 mm2/sec. (D) Photomicrograph of hematoxylin and eosin (H&E) staining (×10) shows invasive adenocarcinoma, with high magnification (×100) images showing the acinar pattern (E) and papillary pattern (F).
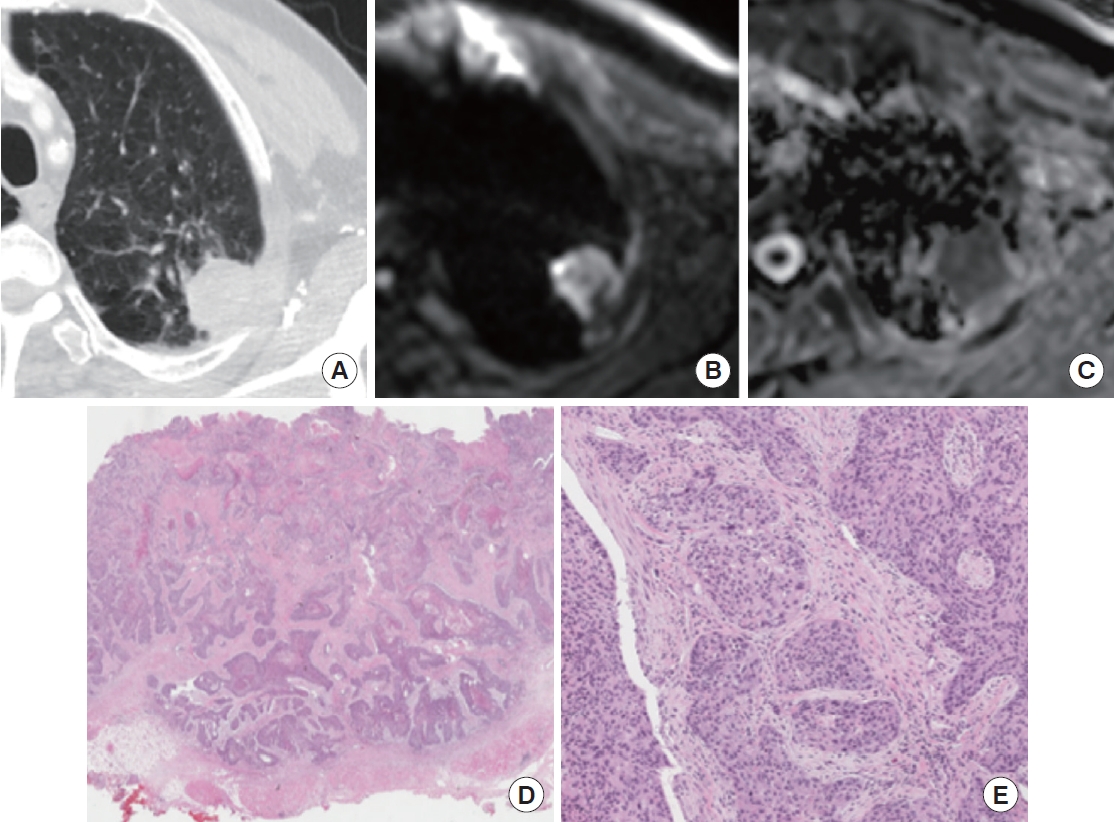
Case of a 74-year-old male with squamous cell carcinoma in the left upper lobe. (A) Conventional computed tomography shows a well-defined nodule in the left upper lobe. (B) Diffusion-weighted imaging (b-value=700) shows a high signal. (C) The mean apparent diffusion coefficient of the carcinoma was 0.979×10−3 mm2/sec. (D) Photomicrograph of hematoxylin and eosin (H&E) staining (×10) shows squamous cell carcinoma, (E) with high magnification (H&E, ×100) showing that the moderately differentiated squamous nodule contains nests of polygonal cells.
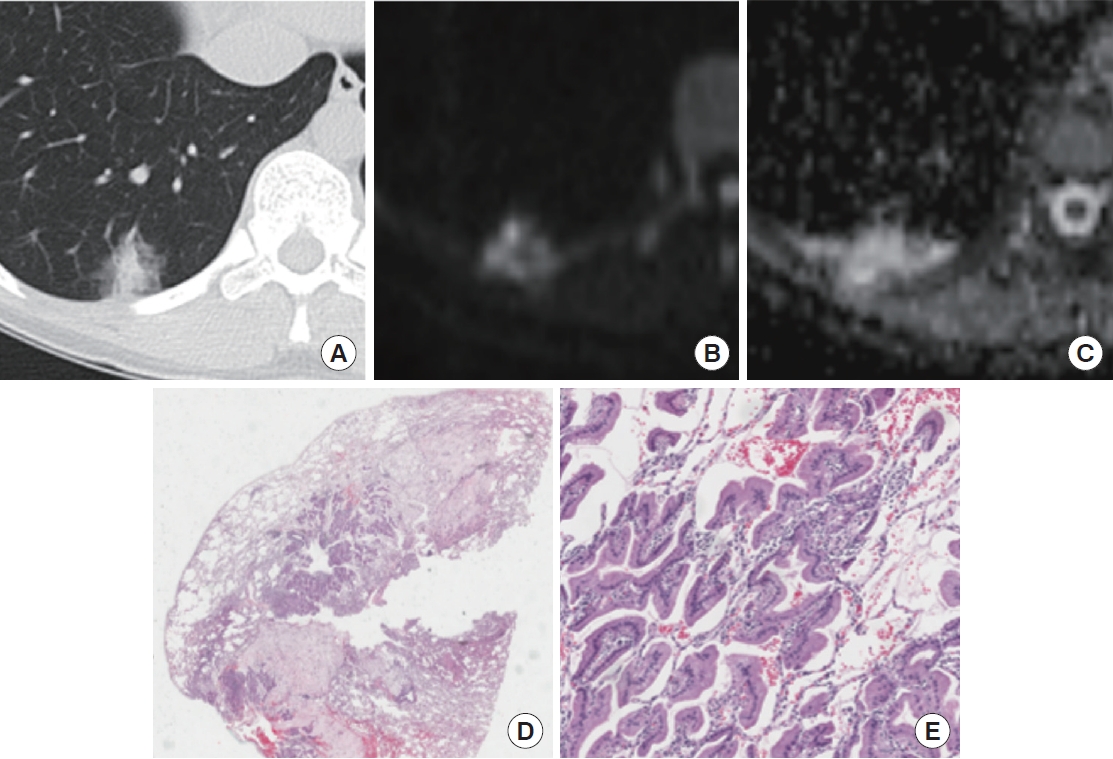
Case of a 40-year-old female with mucinous adenocarcinoma in the right lower lobe. (A) Conventional computed tomography shows a part-solid nodule in the right lower lobe. (B) Diffusion-weighted imaging (b-value=500) shows a high signal. (C) The mean apparent diffusion coefficient of the carcinoma was 3.453×10−3 mm2/sec. (D) Photomicrograph of hematoxylin and eosin (H&E) staining (×10) shows invasive mucinous adenocarcinoma, (E) with high magnification (×100) showing the cuboidal tumor cells with abundant cytoplasmic mucin.
As for CEST imaging, APT-weighted imaging appears to be as useful as DWI and FDG-PET/CT for differentiating between malignant and benign nodules [35]. Although ADC sensitivity was significantly higher than that of magnetization transfer ratio asymmetry (3.5 ppm) and maximum standardized uptake value (SUVmax), its specificity was significantly lower (P<0.05) [35].
Lung cancer staging
Accurate staging based on primary tumor and regional lymph node features and the presence of metastasis is an important step in determining appropriate management and predicting lung cancer prognosis [109,110].
T descriptor
Although CT has been used as the standard reference for lung cancer T-staging, it has limited value in evaluating tumor invasion into adjacent structures because of relatively low soft tissue contrast, which can cause underestimation of the T-stage in advanced lung cancer [111]. On the other hand, MRI was earlier proposed to be superior to CT for T-staging evaluations because of its excellent soft tissue contrast and high spatial resolution (Fig. 8) [111-113].

Case of a 63-year-old woman with squamous cell carcinoma in the left upper lobe who underwent a post-salvage left upper lobectomy and en bloc superior segmentectomy of the left lower lobe. (A) Contrast-enhanced computed tomography images showing a 35 mm mass around the suture materials in the left lower lobe abutting the descending thoracic aorta (arrow). (B) T1-weighted magnetic resonance imaging (MRI) revealed an isodense mass in the left lower lobe encasing 180-degrees of the descending aorta (arrows). (C) Post-contrast T1-weighted MRI with fat-suppression revealed a heterogeneously enhanced tumor with suspicious invasion of the descending thoracic aorta (arrowhead). (D, E) Microscopic evaluation of the resection specimen obtained after left pneumonectomy stained with hematoxylin and eosin showed the tumor (T*) encasing the aorta (Ao) and (arrows) in the aorta wall (original magnification: D, 40×; E, 400×).
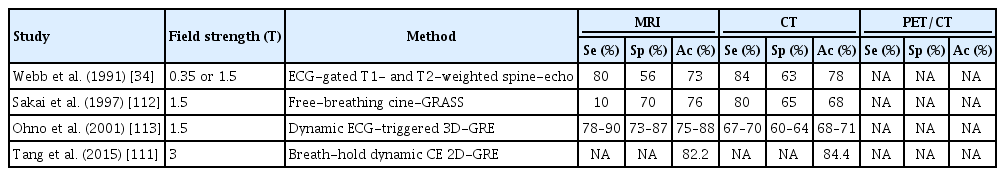
ECG-triggered MR angiography improves image quality by reducing cardiac motion- and breathing-related artifacts in pulmonary vessels and allowing the detection of hilar and mediastinal invasion in lung cancer (sensitivity, 89% to 90%; specificity, 83% to 87%; accuracy, 86% to 88%) [113]. Zhang et al. [114] reported that 3T CE-MRI using free-breathing, fat-saturated, radial VIBE was superior to CT in detecting and distinguishing NSCLC without visceral pleural surface invasion (VPSI) from that with VPSI (sensitivity, specificity, and accuracy: 83%, 95%, and 91%,respectively). Moreover, MRI is superior to CT in evaluating brachial plexus invasion of superior sulcus tumors and is used as the reference standard (Fig. 9) [115]. One study showed that CE-T1-weighted fat-suppression and T2-weighted fat-suppression were the most sensitive sequences for evaluating vertebral invasion of superior sulcus tumors [116];therefore, MRI is useful for pre-operative T-staging in advanced lung cancer, offering excellent soft tissue contrast. Another study showed that MRI was slightly superior to multi-detector CT in advanced-stage NSCLC T-staging, whereas multi-detector CT was more accurate for early-stage tumors [111]. Table 5 shows the reported diagnostic performance of MRI for lung cancer T-staging.
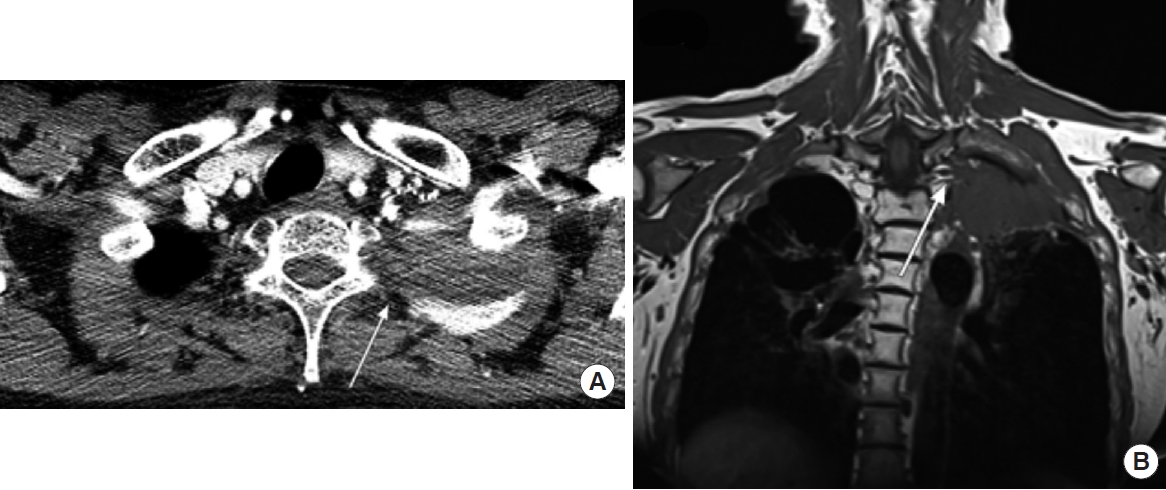
A superior sulcus tumor in a 48-year-old man with left shoulder pain. (A) Axial computed tomography image shows a superior sulcus tumor in the left lung apex. The mass abuts the T1 vertebral body (arrow), but the presence or degree of any extension into the foramen is difficult to determine. (B) Coronal T1-weighted magnetic resonance imaging revealed that the left superior sulcus invaded the distal brachial plexus of the T1 nerve (arrow). As invasion of the brachial plexus indicates tumor unresectability, the patient underwent concurrent chemoradiation therapy.
N descriptor
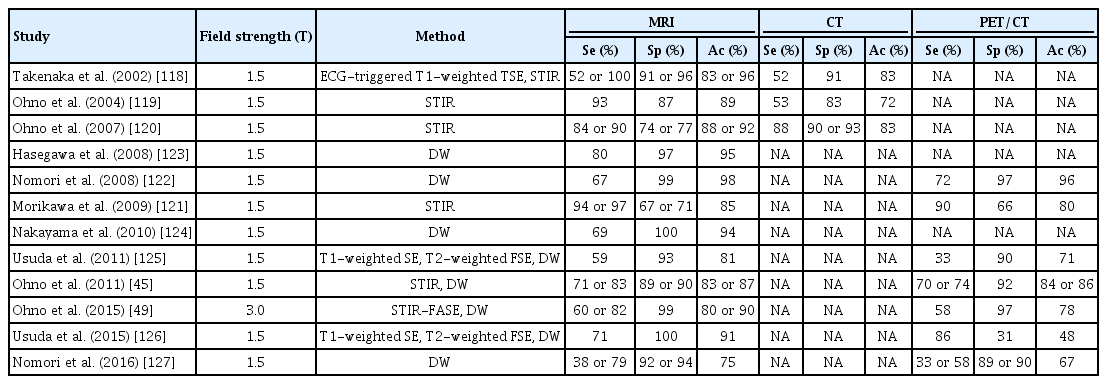
Accurate N-staging is of utmost importance when choosing an appropriate treatment strategy. Differentiating between metastatic and non-metastatic lymph nodes depends on the size and shape criteria used with MRI and CT. A meta-analysis demonstrated the high diagnostic performance of MRI for N-staging in NSCLC on both a per-patient and per-node basis, supporting the clinical relevance of MRI for N-staging in NSCLC [11,117]. Table 6 [45,49,118-127] shows the diagnostic performance of thoracic MRI for lung cancer N-staging. STIR TSE imaging and DWI are also useful for determining the N descriptor in NSCLC [13]. STIR TSE images enhance the net tissue contrast for malignant lymph nodes compared with benign lymph nodes as T1 and T2 relaxation times increase [45]. STIR TSE imaging can also be useful for N-staging in NSCLC, with equal or higher sensitivity (83.7% to 100%), specificity (70.9% to 93.1%), and accuracy (84.7% to 92.2%) than CT, FDG-PET, and PET/CT [118-121]. DWI is another promising MR technique for distinguishing between metastatic and non-metastatic lymph nodes (Fig. 10) [122] (sensitivity, specificity, and accuracy: 83.7%–100%, 74.4%–96%, and 79.5%–95%, respectively) equal to or higher than those for FDG-PET and PET/CT [49,122,123,128,129]. Two meta-analyses reported that the sensitivity and specificity of DWI were 0.72 and 0.95–0.97 and those of FDG-PET/CT were 0.65–0.75 and 0.89–0.93,respectively [130,131].
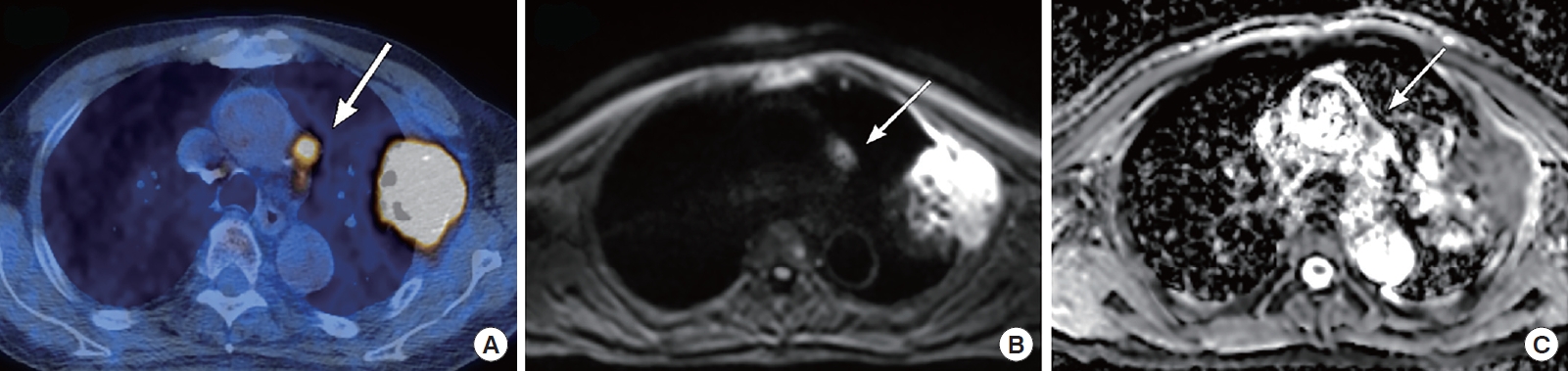
Case of an 80-year-old man with adenocarcinoma in the left upper lobe. (A) Fused positron emission tomography/computed tomography image clearly showing a malignant subaortic node (arrow). (B) The lymph node depicted in the b=700 diffusion-weighted image (arrow) (C) had low apparent diffusion coefficient (ADC) values in the corresponding, mono-exponential ADC map (arrow). The subaortic node was confirmed as being metastatic based on an endobronchial ultrasound bronchoscopy-guided transbronchial needle biopsy.
M descriptor
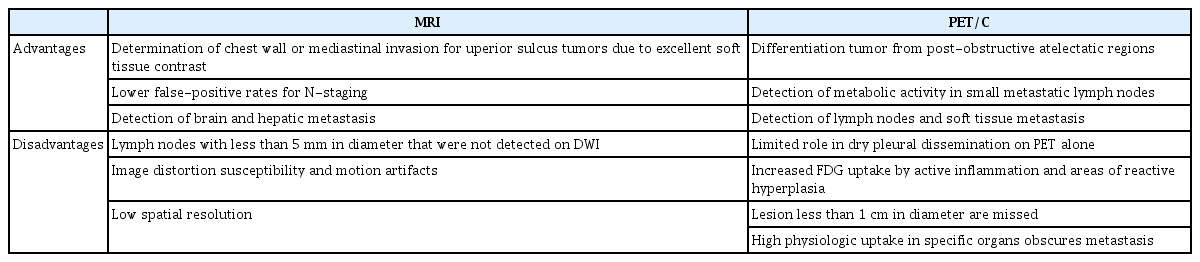
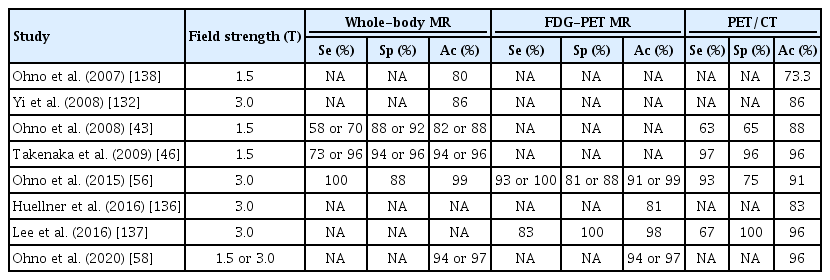
In routine clinical practice, distant metastasis is evaluated using CE-CT, bone scintigraphy, brain MRI, and PET/CT. Whole-body MRI has become clinically feasible and provides acceptable accuracy for NSCLC M-staging compared to PET/CT [6]; it is more useful for evaluating brain and hepatic metastases, whereas PET/CT is useful for detecting lymph node and soft tissue metastases [132]. As MRI provides better contrast than PET/CT, metastases in the brain, liver, and kidney can easily be detected, whereas with PET/CT, metastases can be obscured by physiological uptake [132], which also necessitates additional brain MRI for complete M-staging. Recently, fibroblast activating protein inhibitor (FAPI) tracers that have low uptake in almost all normal tissues, including the brain and bowel, have been developed [133,134]. However, despite the low uptake in the brain on FAPI-PET/CT being a potential advantage over FDG for M-staging [134], false-positives are frequent in bone and liver MRI, because hemangiomas, nodular hyperplasia flow-related enhancement, and marrow signal intensity changes can mimic metastases [132]. Yi et al. [135] used co-registered whole-body MR-PET as a staging tool and found that NSCLC was correctly up-staged in 25.9% and 21.7% of patients in the MR-PET and PET/CT plus brain MRI groups, respectively (4.2% difference, 95% confidence interval [CI], –6.1 to 14.5; P=0.426). Hybrid PET/MR systems have also recently become clinically feasible. The diagnostic accuracy of PET/MR for M descriptor assessment was equal to or higher than that of PET/CT [136,137]. Table 7 shows the reported diagnostic performances of whole-body MRI and PET/MRI for M-staging in lung cancer [43,46,56,58,132,136-138]. The advantages and disadvantages of PET/CT and chest MRI for lung cancer staging are summarized in Table 8.
Prediction of post-operative pulmonary function
Approximately 90% of lung cancer patients have underlying chronic obstructive pulmonary disease (COPD) or cardiovascular disorders, which are associated with a high-risk of intraoperative and post-operative complications [139]. As COPD patients show regional differences in pulmonary function because of lung tissue destruction, it is important to assess these in pre-operative evaluation for lung resections in such patients [140]. Spirometry, CT, and nuclear medicine-based examinations are standard pre-operative evaluations for patients undergoing lung resection [141]. Recently, various MRI techniques have been used to predict post-operative lung function. 3D DCE-perfusion MRI is a useful new technique for evaluating regional pulmonary perfusion and assessing a patient’s physiological and pathological conditions [142], showing superiority to qualitatively assessed pulmonary perfusion scintigraphy, CT, and single-photon emission CT [141,142]. The correlation between actual post-operative forced expiratory volume in 1 second (FEV1) and post-operative FEV1 predicted using 3D DCE-perfusion MRI is excellent [141,142]. One study reported that the post-operative FEV1 predicted using non-CE perfusion MRI with the fresh blood technique correlated significantly with actual post-operative FEV1 (r=0.98) [143]. Non-CE perfusion MRI is a technique for evaluating post-operative lung function in patients with contraindications for gadolinium contrast agent use [13]. Oxygen-enhanced MRI is another potential approach for imaging pulmonary ventilation [144]. A study showed an excellent correlation between the FEV1 predicted using oxygen-enhanced MR and actual post-operative FEV1 (r2=0.81) [145].
Post-operative lymphatic leakage evaluation
The use of aggressive surgical techniques for improving the curability of patients with cancer may contribute to increased post-operative lymphatic leakage. Several studies have reported that post-operative chylothorax often occurs after pneumonectomy (0.37%) and lobectomy (0.26%–2.3%) [146-148]. For patients with persistent high-output chylothorax for whom conservative dietary treatment has failed, re-operation to ligate the thoracic duct is necessary [149,150].
The most popular traditional imaging modality for lymphatics is scintigraphy, but it has poor spatial resolution [151,152]. Direct lymphangiography requires cannulation of peripheral lymphatic channels and infusion of an oil-based contrast agent. Catheterization of small lymphatic channels can be problematic, and significant respiratory complications can occur due to pulmonary oil embolisms or pneumonitis [153]. Invasive CT or MR lymphangiography (MRL) (Fig. 11) is also incredibly challenging because image acquisition requires the difficult intervention of an intranodal injection. [154] Conversely, intrinsic contrast can be used for non-invasive MRL [155]. Due to the variations in the central lymphatic structure [156], it is critical to visualize the structure as well as the leakage point for both accurate diagnosis and therapeutic planning [157]. The termination site of the thoracic duct is another feature that needs to be visualized well, because it is where lymphatic leakage often develops, and it is related to supraclavicular lymph node dissection. In addition, when the interventional approach from the femoral side fails, interventional radiologists have to attempt the procedure from the subclavian side, and lymphangiography, particularly for that portion, provides very helpful guidance.
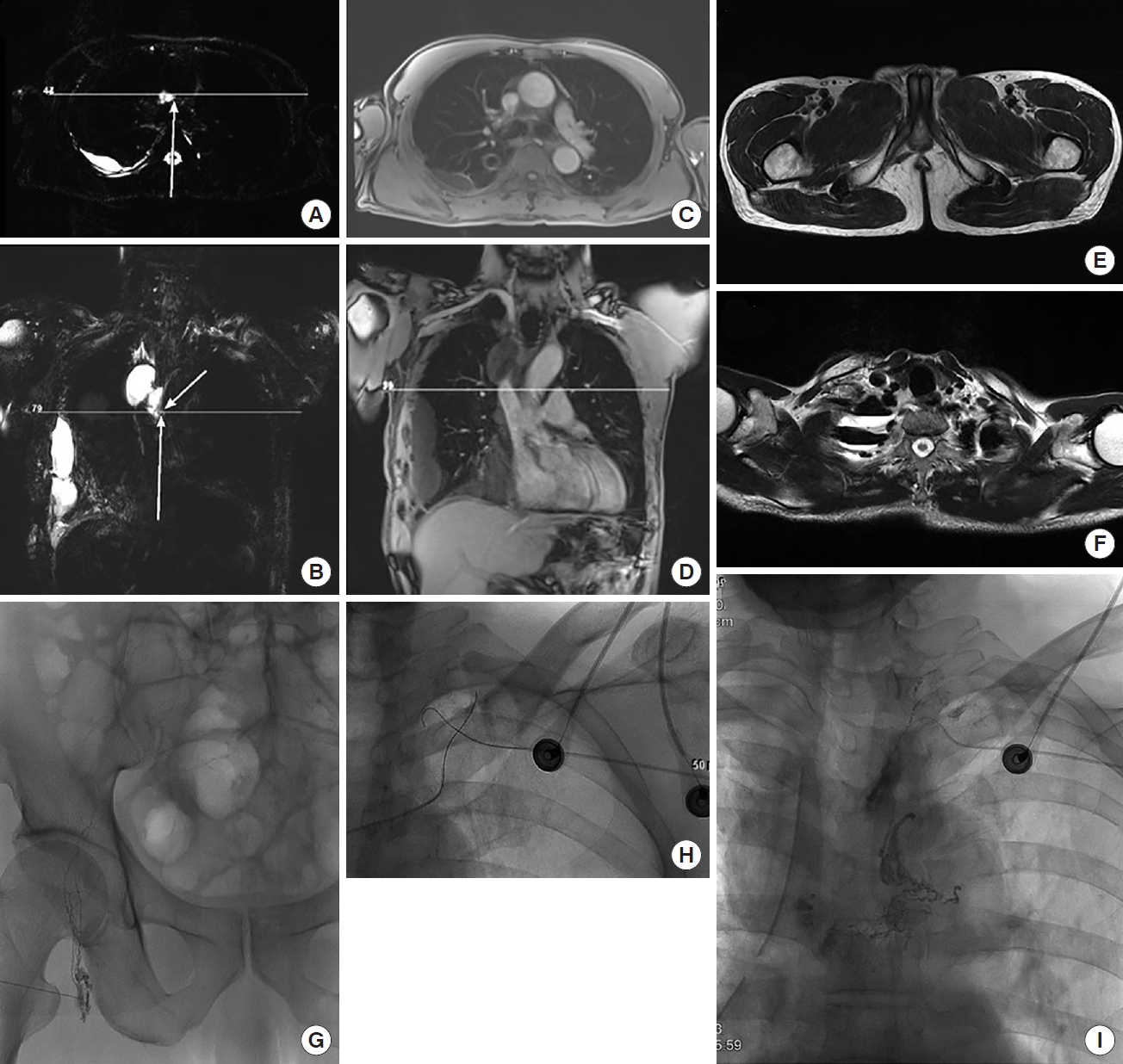
Images from a representative protocol for non-invasive magnetic resonance (MR) lymphangiography. (A, B) Axial and coronal lymphangiography plane images obtained using a heavily T2-weighted sequence, all with free-breathing status. Lymphangitic leakage (arrows) was suspected at the carina level. (C, D) Fast enhanced images based on a 3D gradient-recalled-echo T1-weighted sequence for obtaining anatomical information. (E, F) T2-weighted images without fat-suppression of the inguinal and periclavicular areas for possible follow-up interventions such as thoracic duct embolization. (G) Lymphatic leakage was suspected at the left side of the carina; therefore, fluoroscopic lymphangiography with the inguinal approach was attempted, but was unsuccessful. (H) A second attempt with the sub-clavicular approach using T2-weighted imaging followed, and contrast leakage was observed at the same site as in the MR lymphangiography image (I).
Two important factors should be taken into account for MRL. First, free-breathing should be considered, because lung cancer is frequently diagnosed in elderly patients who find it difficult to hold their breath during acquisition; additionally, lung cancer patients experience significant post-operative dyspnea. Second, the ingestion of 1 to 3 tablespoons of olive oil is quite useful for improving the quality of lymphangiography images, because it stimulates lymphatic flow [158].
One recent study compared the performance of intranodal lymphangiography and thoracic duct embolization with that of MRL in 50 patients with post-operative chylous leakage in terms of diagnosing leakage and imaging the anatomic details of the lymphatic structures (Fig. 12) [157]. The sensitivity, specificity, and positive and negative predictive values of MRL for leakage detection were 100%, 97.1%, 100%, and 100% respectively, and its concordance rate was 97.14% (95% CI, 85.08 to 99.93; P<0.001).
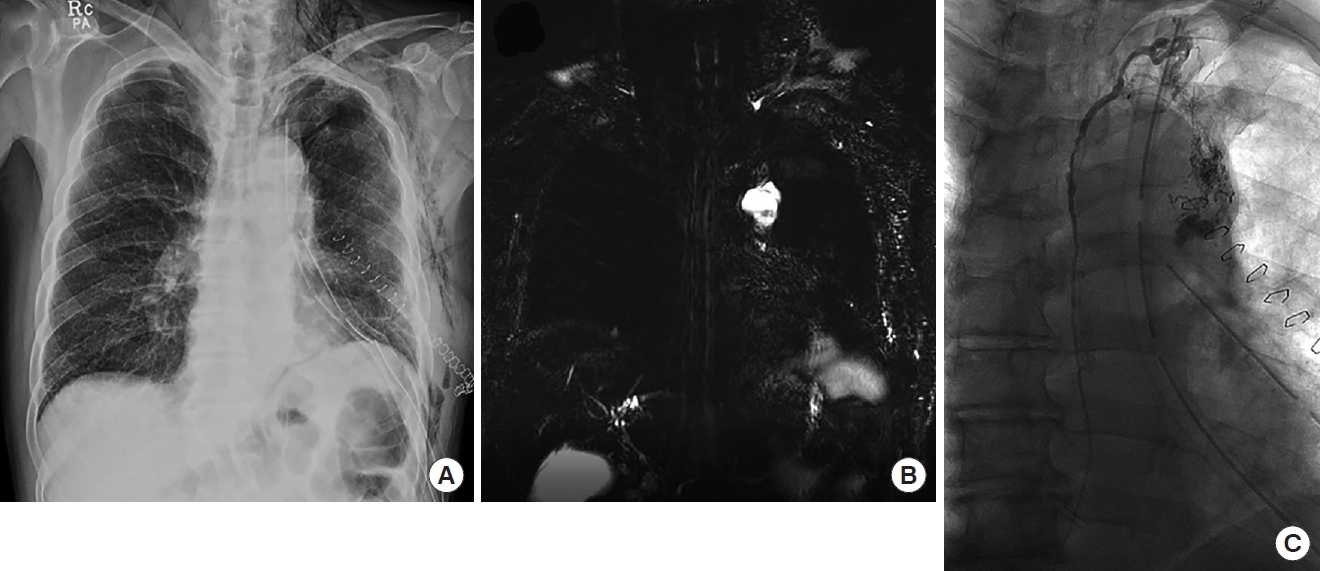
(A) A case of chylothorax at post-operative day 5 after left upper lobe lobectomy for lung adenocarcinoma. Magnetic resonance lymphangiography (B) revealed an abnormal fluid pocket at the superior aspect of the aortic arch, and a connection to the subclavian part of lymphatic system was noted. Fluoroscopic lymphangiography (C) revealed lymphatic leakage at the corresponding point, which could have been due to a lymphatic injury during para-aortic lymph node dissection.
Treatment response evaluation
MRI can be a problem-solving tool during treatment response evaluation, for example, in differentiating between radiation pneumonitis and true progression. Radiation-induced pneumonitis is quite non-specific and sometimes obscures tumor recurrence. According to an article by Jagoda et al. [159], 12 patients with NSCLC stages I–III who were scheduled for radiochemotherapy underwent CE-CT and non-enhanced MRI before and 3, 6, and 12 months after treatment. No significant difference was observed in longitudinal diameter or tumor volume between MRI and CT, and the ADC value for detecting residual malignancy or recurrence was more sensitive than CT because non-responder lesions had significantly lower ADC values than those of responders.
When using CT for cancer patients, the downside of the recent exponential increase in CT and MRI use is that a sizable proportion of patients experience side-effects due to contrast agents. When these side-effects were categorized into five subgroups based on involved organ and severity, the incidence of severe adverse reactions was quite high [160-163]. However, advanced lung cancer patients must undergo follow-up imaging, regardless of adverse reactions. As MRI requires little or no contrast agent use, patients experiencing severe adverse reactions to CT contrast agents could use MRI as a surveillance imaging modality instead (Fig. 13).
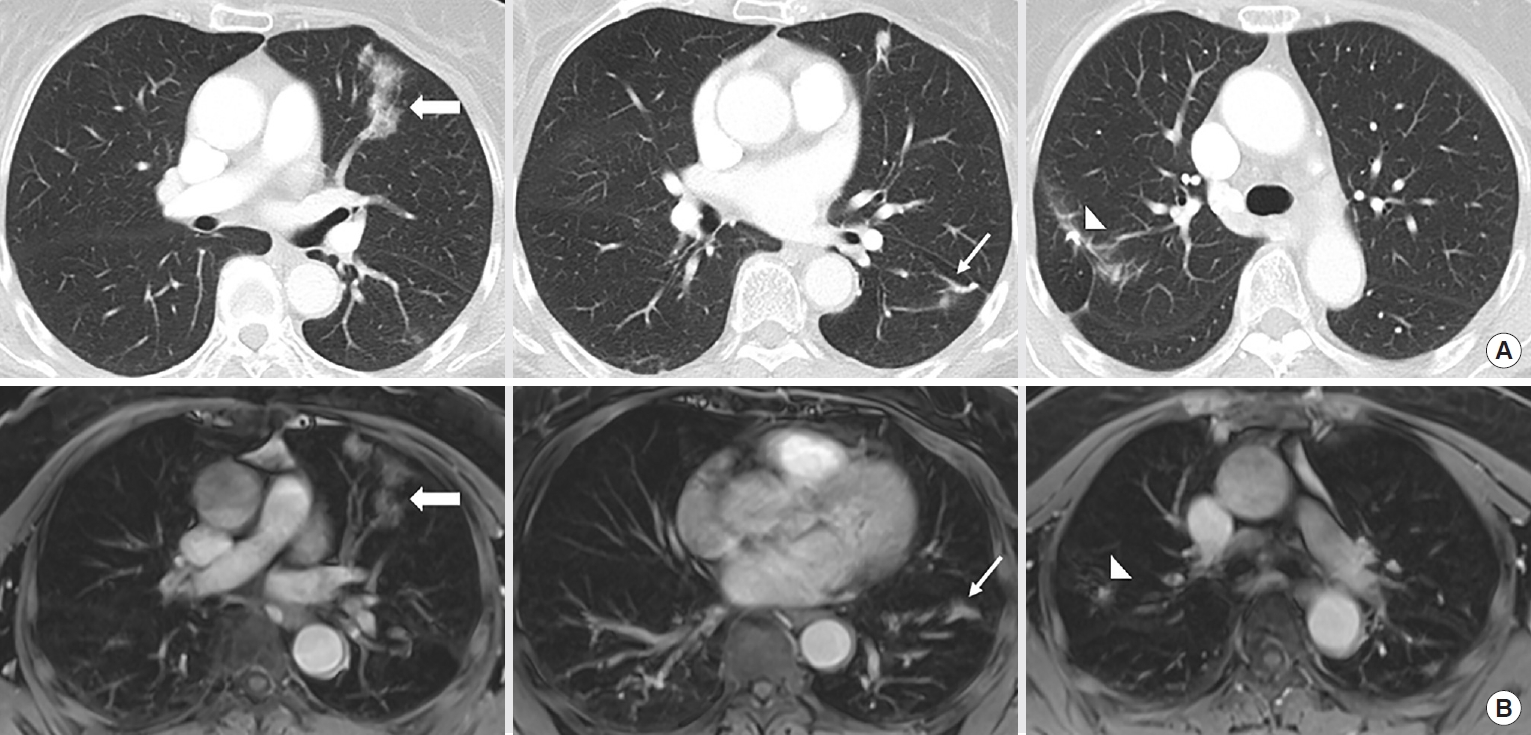
A 60-year-old male who had undergone right upper and left lower wedge resections for adenocarcinomas. Magnetic resonance imaging was conducted at the 3-month follow-up due to an adverse reaction to the contrast agent. (A) Contrast-enhanced computed tomography images show ground glass opacity in the left upper lobe (thick arrow), with post-operative changes in the left lower lobe (thin arrow) and right upper lobe (arrowhead). (B) Ground glass opacity in the left upper lobe (thick arrow) and post-operative changes in the left lower lobe (thin arrow) and right upper lobe (arrowhead) are also visible on contrast-enhanced T1-weighted gradient-recalled-echo images with fat-suppression.
For more precise treatment evaluations, multimodal analysis using PET and DWI can be considered [164]. By integrating SUVmax and ADC values, we divided the entire tumor volume into four subregions, including necrotic areas and areas indicating high tumor aggressiveness (Fig. 14). Focusing the resulting partitioning-based clustering on highly aggressive areas showed better predictive performance for overall survival than whole tumor volume or voxel-based approaches (Fig. 14).
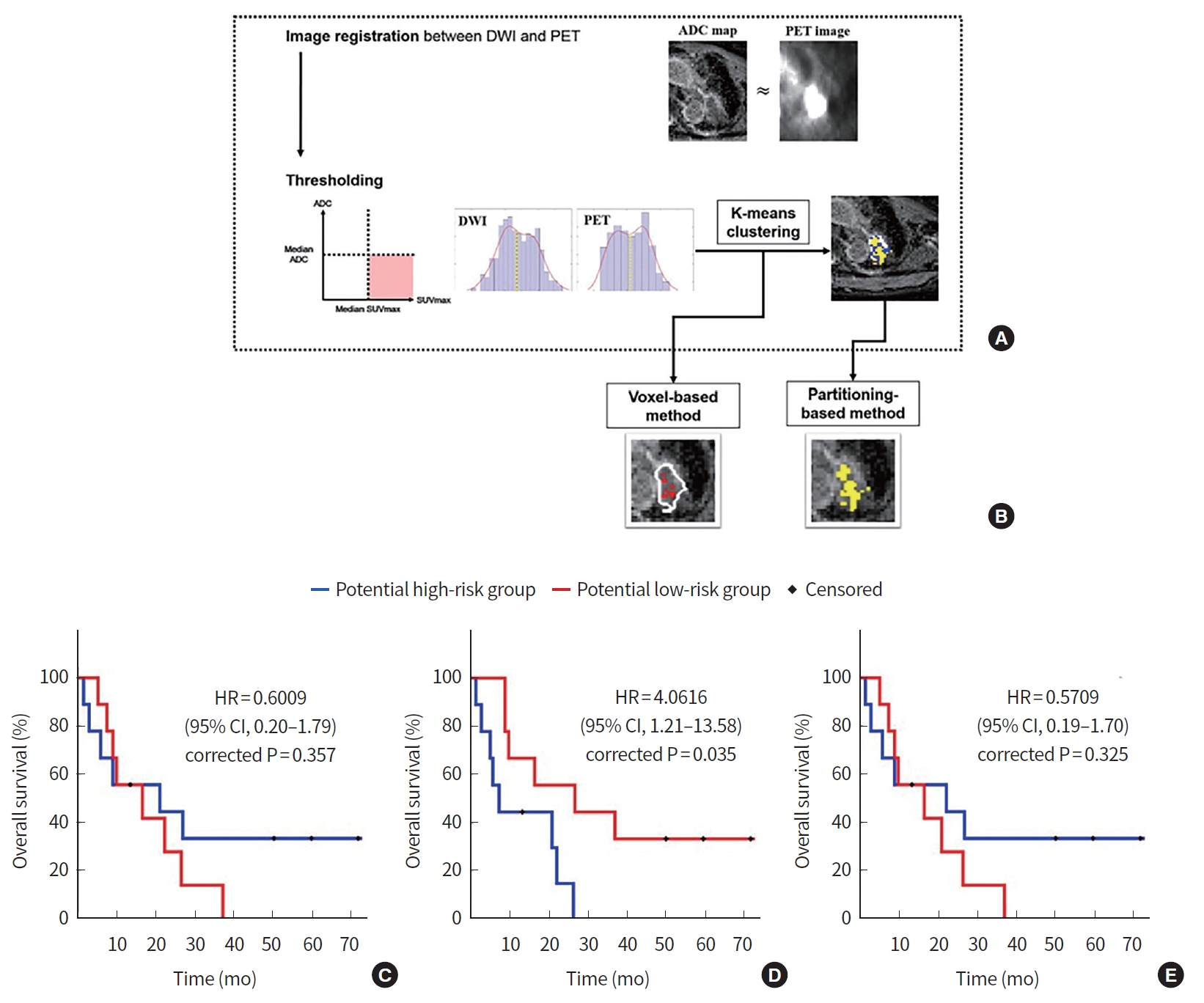
Multimodal analysis using positron emission tomography (PET) and diffusion-weighted imaging (DWI). (A, B) Overview of the image processing steps. Overall processing includes two parts. Panel (A) involves PET and DWI image registration, thresholding against median values, and k-means clustering. Panel (B) involves computing the hot spot using a voxel-based method (left, using the threshold rule only) and a partitioning-based method (right, using both the threshold rule and clustering). (C, D, E) Results of survival analyses. (C) Kaplan-Meier plot for the whole tumor volume approach. (D) Kaplan-Meier plot for the partitioning-based approach. (E) Kaplan-Meier plot for the voxelwise approach. Reprinted from Kim et al. [164], with permission from Springer Nature. ADC, apparent diffusion coefficient; HR, hazard ratio; CI, confidence interval.
FUTURE DIRECTIONS
A biomarker is a characteristic that can be measured objectively to indicate normal biological processes, pathological changes, or response to an intervention [165]. Biomarkers can include molecular, histological, radiographic, and physiological characteristics. In terms of imaging,they can include anatomical, functional, and molecular characteristics [166]. Although CT remains the principal imaging tool for routine pulmonary imaging examinations, MRI has emerged as the clinical standard and has shown enormous potential to transform clinical care for certain patients and indications. In addition, the unique information that current MRI tools provide can be used for mechanistic, hypothesis-driven research in clinical as well as pre-clinical models [6].
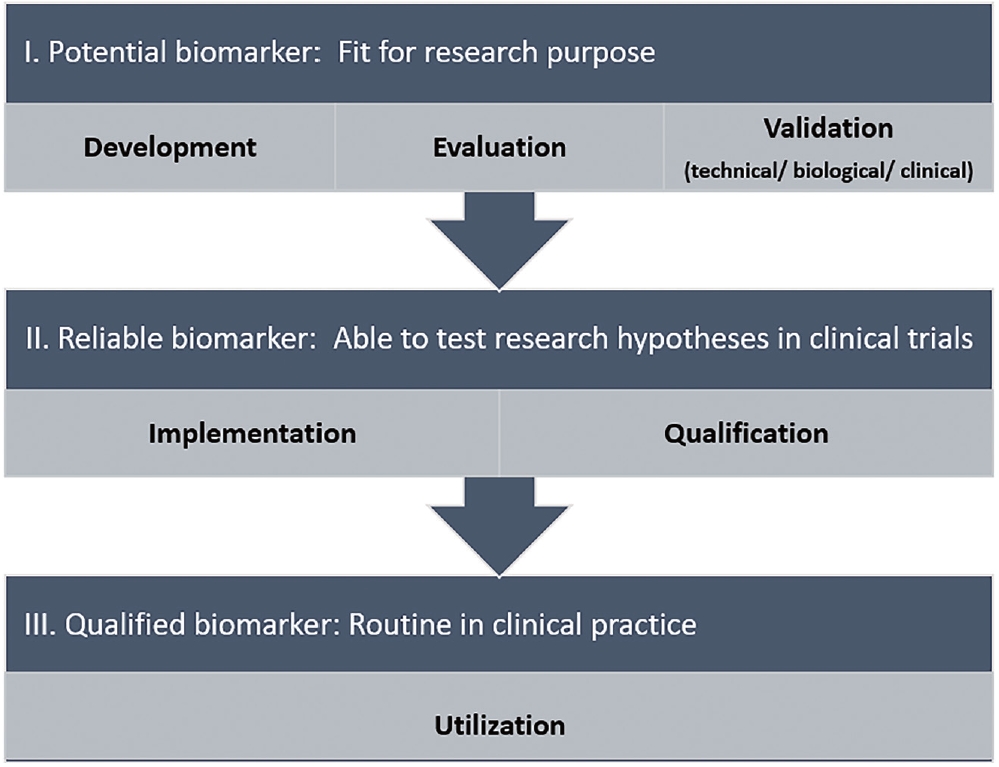
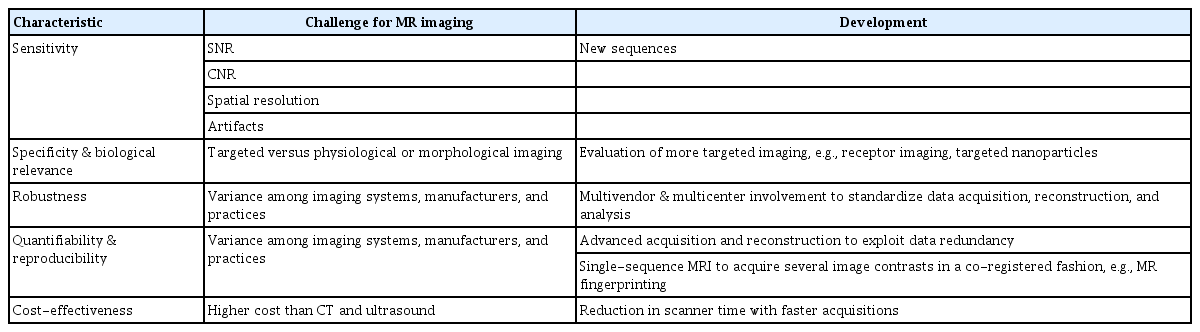
To develop new imaging biomarkers, several steps, often parallel and complementary to one another, need to be undertaken for translation to clinical practice. These can be categorized into the following phases: discovery, development and evaluation, validation, implementation, qualification, and utilization. These phases must also cross two translational gaps, to patients and into practice (Fig. 15) [167]. MRI has many advantages, including superior soft tissue contrast and high spatial resolution, the potential of the use of multiple contrasts in a single examination, and its ability to allow assessment of physiological processes such as vascularization, oxygenation, and diffusion [167]; nevertheless, there are several key characteristics and challenges in using MRI biomarkers (Table 9).
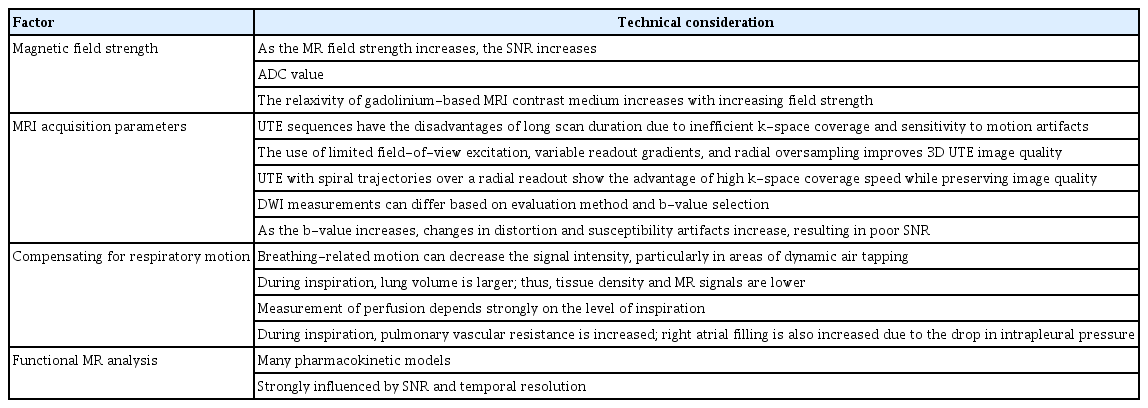
When considering more advanced applications of full-fledged MRI biomarkers, we first need to consider how to obtain high-quality MR data after removing various artifacts (Table 10) [168]. Table 11 lists the vital elements required to maintain technical reproducibility [169].
Most thoracic MRI examinations are performed to answer a specific clinical question that originates during the interpretation of a prior CT or PET examination. Consequently, most thoracic MRI examinations can be tailored to the patient and the clinical questions being addressed in a practical example of personalized medicine. For example, Raptis et al. [170] proposed creating thoracic MRI protocols using five questions (Fig. 16).
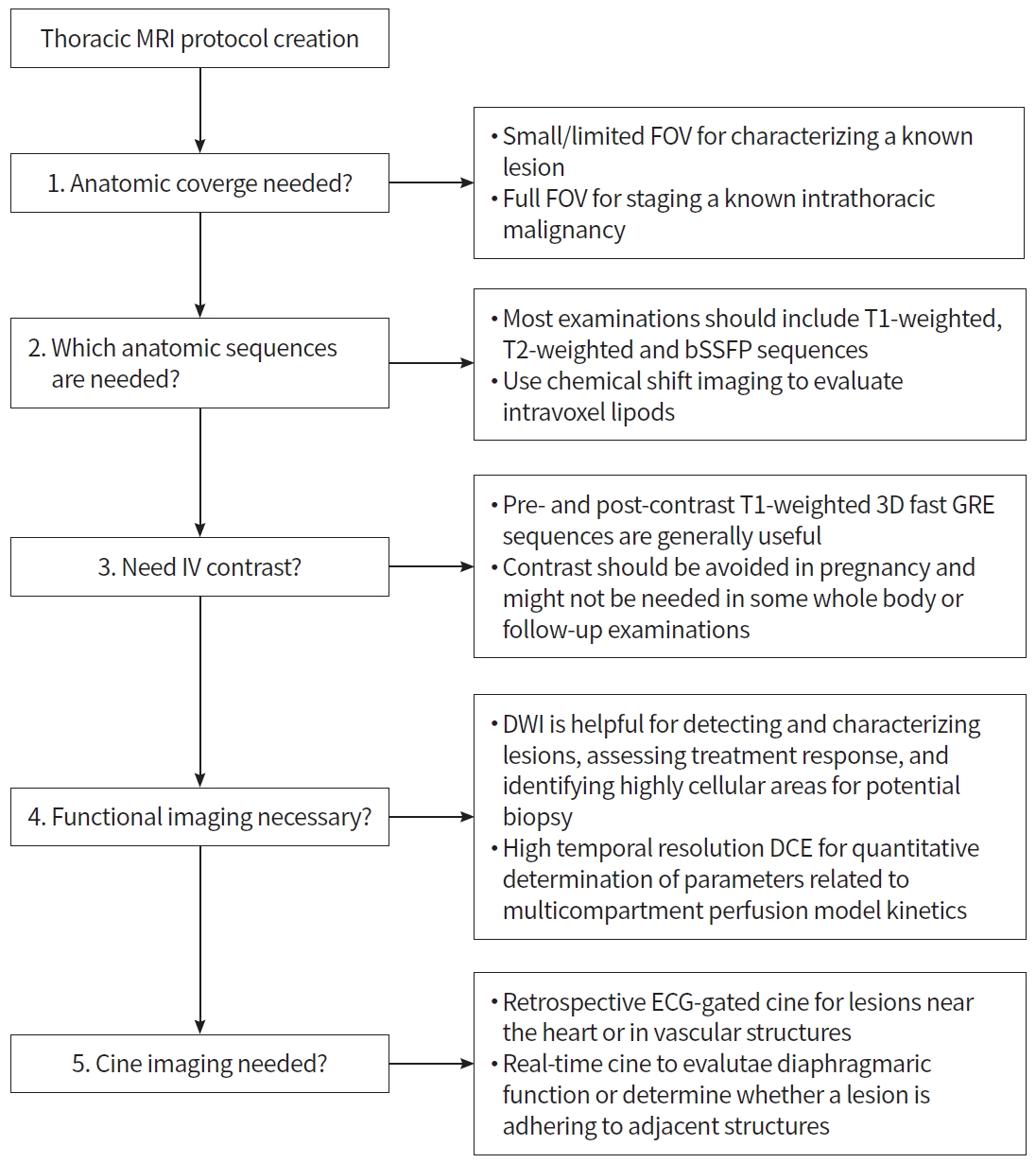
Building blocks for thoracic magnetic resonance imaging (MRI): challenges, sequences, and protocol design [170]. FOV, field-of-view; bSSFP, balanced steady state free precession; IV, intravenous; GRE, gradient-recalled-echo; DWI, diffusion-weighted imaging; DCE, dynamic contrast-enhanced; ECG, electrocardiogram.
Compressed sensing (CS) is an alternative acceleration technique that exploits the inherent sparsity of MRI to reconstruct images by under-sampling k-space data [171]. In contrast to parallel imaging, CS does not require the use of multiple-channel radiofrequency coils, facilitating the translation of the technique across different sites and scanners. Three requirements must be satisfied to ensure good CS image reconstruction: (1) image data must be sparse in either the image domain or a transform domain; (2) the k-space must be randomly under-sampled with variable-density schemes to ensure that the associated artifacts produced during reconstruction are incoherent/noise-like and can be smoothed using the CS algorithm; and (3) a non-linear reconstruction method must be used to enforce sparsity and data fidelity [172]. The reduction in acquisition time offered by CS allows isotropic resolution of 3He and 1H lung MR images acquired in the same breath-hold [173]. CS techniques have also been implemented to enable high temporal resolution gas flow measurements in the upper airways with phase-contrast velocity [174]. The development of these key methods facilitated the clinical translation of this technique for the evaluation of multiple aspects of lung function in several pulmonary disorders.
Artificial intelligence (AI) in imaging has also made great strides in the past few years. AI-based systems are used for tasks that are typically performed by diagnostic radiologists, such as scan quality evaluation, whole lung/nodule segmentation, lesion detection, and disease classification in research settings [175,176]. However, the majority of research-based AI solutions aiding these steps require training with large, diverse datasets, and the AI models need to be tested in real-life settings before routine use in clinical practice.
CONCLUSION
Until recently, the clinical use of thoracic MRI was limited. However, advanced methods are expanding the opportunities to exploit the advantages of MRI in the evaluation of several common lung disorders. MRI helps to visualize structural and functional lung abnormalities without the need for ionizing radiation, making state-of-the-art MRI techniques an alternative to CT, particularly for pediatric patients, women of child-bearing age, pregnant women, and patients requiring serial follow-up imaging [6].
Multiple challenges remain to be addressed in incorporating pulmonary MRI into routine clinical practice. These include further validation of image-based measures, standardization of image acquisition and analysis, establishment of normal values, demonstration of cost-effectiveness and improved patient outcomes, efficient integration into radiology workflows, and regulatory approval of investigational techniques [4]. Interdisciplinary collaboration between clinicians and scientists with expertise in oncology, imaging, and physiology is needed to address these challenges and prioritize the most useful clinical applications that can expand the role of thoracic MRI in the evaluation and treatment of lung cancer patients.
Notes
No potential conflict of interestrelevantto this article was reported.
AUTHOR CONTRIBUTIONS
Conception or design: HYL.
Acquisition, analysis, orinterpretation of data: SHB, CK, CHK, HYL.
Drafting the work orrevising: SHB, CK, CHK, YO, HYL.
Final approval ofthe manuscript: SHB, CK, CHK, YO, HYL.
Acknowledgements
This work was supported by Future Medicine 20*30 Project of the Samsung Medical Center (#SMX1210781) and the National Research Foundation of Korea (NRF) grant funded by the Korea government(MSIT) (NRF-2021R1A4A5032806).